Healthcare Solutions
Working with hospitals to ensure patients have fewer delays and lessen the risks of getting sicker at the place that is meant to make you better

Patient Safety
Arrowsight RVC services provide direct observation in the hospital setting and help Providers raise their adherence to hospital protocols resulting in a safer environment for their patients.
Whether we are auditing in the Operating Room, the hospital wards, or the sterilization rooms – Arrowsight RVC provides feedback directly to the providers helping them to improve the environment for patients.
Surgical safety checklist
Hand Hygiene Compliance
PPE Donning & Doffing

Environmental Services/ Cleaning
Arrowsight’s auditing services have been shown to increase compliance for a variety of complicated and detailed procedures.
Room Cleaning
Endoscope Reprocessing
OR Attire Compliance

Patient Flow/Throughput
Near Real-Time video auditing provides prompt feedback and relevant metrics to increase utilization in operating rooms and emergency departments.
Operating Room Efficiency
Arrowsight RVC helps to improve Operating Room Efficiency by providing feedback to clinical teams.
ED Admits to Hospital
Helping to improve the time an admitted patient receives an in-pateint hospital bed
Healthcare Studies & Publications
There are many sources of contamination in the perioperative environment. Patient experience can be negatively affected by the presence of environmental contamination, especially if it is the cause of a surgical site infection. Perioperative and environmental services staff members and leaders are tasked with ensuring a clean and safe environment for their patients while maintaining an awareness of time and budgetary constraints. In addition, leaders are responsible for the competency of their staff members and must address performance issues when needed. New technological advances designed to streamline monitoring and reporting processes related to OR cleanliness are available for use. This article describes the quality improvement project that one multifacility organization completed related to the use of remote video auditing and the positive effect it had on the organization’s environmental contamination.
Implementation of remote video auditing with feedback and compliance for manual-cleaning protocols of endoscopic retrograde cholangiopancreatography endoscopes
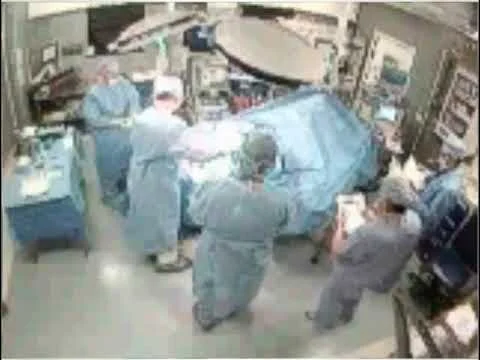
Remote Video Auditing in the Surgical Setting
Remote video auditing, a method first adopted by the food preparation industry, was later introduced to the health care industry as a novel approach to improving hand hygiene practices. This strategy yielded tremendous and sustained improvement, causing leaders to consider the potential effects of such technology on the complex surgical environment
Transparency can be a powerful driver of better healthcare quality. In 2013, it was proposed that recording video data in healthcare begin with the several medical procedures that are already video based (cardiac stent placement, arthroscopic surgery, colonoscopy, etc). Different from the past era when recording required new hardware, most of the procedures performed in medicine today are now mediated by video, enabling a new opportunity for learning health systems.
The operating room (OR) is a complex system that requires a carefully coordinated workflow to ensure both safe and efficient operation. Video monitoring of ORs has been described on a small scale by Hu who recorded 10 operations and used the video offline to identify and analyse safety and efficiency deficits. Makary discussed the potential of video recording in driving surgical quality improvements and eliminating surgical ‘never events’ as well as the importance of effective teamwork in driving patient safety. The use of a surgical safety checklist has been shown to reduce mortality and complication rates
One method being investigated to increase compliance to cleaning protocols is remote video auditing with near real-time feedback. We evaluated technician compliance with endoscope cleaning and sterilization protocol with the use of remote video auditing with and without feedback.
Ongoing Discovery of High-Level Disinfection of Endoscope Practices and the Use of Performance Improvement Methodologies to Improve Processes
Preventing health care–associated infections, regardless of the setting (hospital, ambulatory, office-based), has become a priority. This focused attention can be attributed to leaders motivated to improve the quality of care with highly reliable, repetitive, evidence-based process practices; patient expectations of an uncomplicated health care experience; increased awareness of reported infections; and financial implications (positive and negative) to the organization
Hand hygiene is a key measure in preventing infections. We evaluated healthcare worker (HCW) hand hygiene with the use of remote video auditing with and without feedback.
Press Release:
North Shore University Hospital Study Demonstrates Hand Hygiene Rates Improve Exponentially When Remote Video Auditing Technology Provides Continuous Feedback to Health Care Professionals Hand Hygiene is Critical to the Reduction of Hospital-Acquired Infections
Objective performance data for processes essential to patient safety and OR efficiency, such as surgical time out (STO), OR cleaning, and OR throughput, are challenging to obtain. When collected by OR stakeholders, these metrics are often biased and time consuming to collect. Video auditing has been described in the OR and beyond to improve the quality of care by influencing behavior, analyzing adverse events, and encouraging best practice.
In Medicine, the problems of wide variations in quality and poor compliance with evidence-based care are well known. More education is not the solution for these problems. Knowledge is abundant, but implementation of knowledge often lags. This Viewpoint explores whether use of an existing technology, video recording of medical procedures, can improve quality of care
Perioperative services leaders seeking to improve safety and efficiency without sacrificing quality may want to turn to remote video auditing, which is being successfully used in hospital ORs and ambulatory surgery centers.
Preventing health care–associated infections, regardless of the setting (hospital, ambulatory, office-based), has become a priority. This focused attention can be attributed to leaders motivated to improve the quality of care with highly reliable, repetitive, evidence-based process practices; patient expectations of an uncomplicated health care experience; increased awareness of reported infections; and financial implications (positive and negative) to the organization. A topic that has recently become a main concern is high-level disinfection (HLD) and endoscopes used for endoscopic retrograde cholangiopancreatography (ERCP) procedures, as represented in the Food and Drug Administration (FDA) Safety Communication in February 2015.
Faced with an Ebola-related mandate to regularly train front-line hospital staff with the donning and doffing of personal protective equipment, a community hospital’s emergency department implemented remote video auditing (RVA) to assist in the training and remediation of its nursing staff. RVA was found to be useful in assessing performance and facilitating remediation.
Prior to this study, remote video auditing (RVA) on health care workers (HCW) hand hygiene was initiated in 1 medical intensive care unit (MICU) at a tertiery hospital. Hand hygiene compliance within that unit went from less than 10% without feedback to a sustained rate that exceeded 85% after feedback.1 The aim of this study was to assess HCW hand hygiene upon entry and exit on a second, adjacent surgical intensive care unit (SICU) with the use of RVA without and with feedback.
A recent survey of peer review studies related to palliative care by the Agency for Healthcare Research and Quality (AHRQ) found that only five of more than 90 studies targeted multiple outcomes measures and relayed data to providers.
The Society of Gastroenterology Nurses and Associates (SGNA) outlines practice standards for manual cleaning of endoscopic retrograde cholangiopancreatography endoscopes before being placed into a automated endoscope reprocessors (AER) between patients to prevent the transmission of pathogens. Since pathogen transmission can be related to improper cleaning of the endoscope between patients this initiative was designed to assess adherence to the multi-step process for manual cleaning of ERCP endoscopes with the use of remote video auditing (RVA).